Since Medicare Hospice coverage was established in 1982, more patients choose hospice for end-of-life care. Hospice care maximizes the quality of life and supports caregivers in the final stages of an advanced, life-limiting disease. It gives the compassionate mind, body, and spirit care to incurable patients.
Once a doctor prescribes hospice care, you may wonder how long a loved person will live. Hospice can aid patients for months or even years, even though some wait until the end. The longer a particular person is at the hospice, the more enjoyment they can enjoy.
How Does a Patient Become Eligible for Hospice Care?

Hospice patients must meet the U.S. Centers for Medicare and Medicaid Services’ enrollment requirements. Private insurance, Medicare, and Medicaid require two physicians to affirm that a patient is unlikely to live beyond six months to qualify for hospice. Physicians may estimate a six-month life expectancy based on many indicators, although some patients live longer.
Alzheimer’s and Dementia Hospice Care’s Role

Hospice caregivers assist with eating, dressing, and other tasks. They teach family caregivers to recognize and treat early discomfort. Social workers, chaplains, and volunteers help hospice caregivers.
Hospice Eligibility

Because dementia patients’ end-of-life prognoses are tough, hospice is underutilized. Doctors can’t predict how long someone with Alzheimer’s will survive due to the complicated relationship between the brain and body.
Medical professionals may discuss the Functional Assessment Staging Test (FAST) scale. Dementia patients’ everyday function and activity abilities are ranked on seven levels.
How Long Do People Usually Stay in Hospice?

Most patients do not enroll in hospice until they are nearing the end of their lives. According to a Journal of Palliative Medicine study, half of hospice patients died within three weeks and 35.7 percent within one week.
12–15% of patients in the trial survived six months or more. In the study, people under 65 were less likely to die within six months.
Men are 88.4% more likely to die within six months than women, at 85.1 percent. Dementia and stroke patients have lower hospice mortality rates than other patients.
Trella Health says that hospice patients spent 77.9 days in 2018, more than the 74.5 days they spent in 2017. The U.S. Centers for Medicare and Medicaid Services talked to many families and found that many wished their loved one had gone to hospice sooner.
Hospice eligibility is limited to six months. Patients are admitted with a six-month life expectancy. However, many patients survive beyond this time and are eligible for hospice or discharge.
Factors Affecting Life Expectancy

People with dementia have different life expectancies. Factors that affect life expectancy or dementia duration include:
- After diagnosis, how does the disease progress?
- Other conditions include motor neuron disease, cancer, and cardiovascular illness.
- The age at which symptoms begin, with individuals over 65 having a reduced life expectancy.
Early Stage Dementia
According to the NIA, dementia varies in severity. Initially, it may minimally influence a person’s everyday functioning, increasing to the most severe stage, where they may be utterly dependent on others.
Dementia has three stages, according to the WHO: early, medium, and late. The stages may overlap and are mild, moderate, and severe. Some people with dementia progress quickly, while others may remain independent for years.
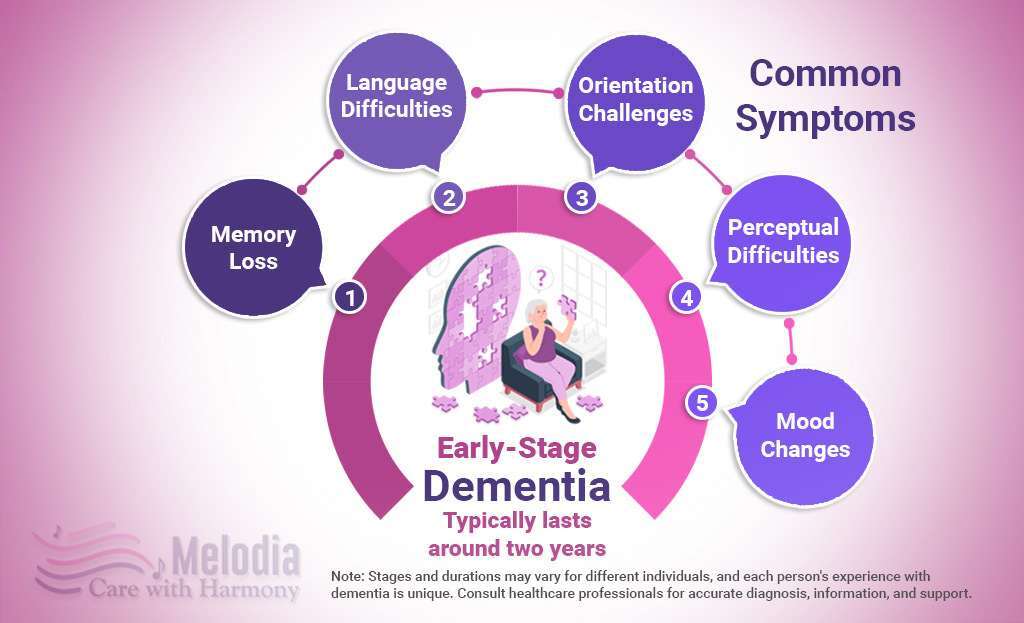
Dementia may last two years in its early stages.
Early Stage Dementia Symptoms Include:
- Memory loss and trouble planning, such as making complex financial decisions.
- Difficulties finding the correct phrases in conversations.
- Poor orientation, such as getting lost in familiar surroundings.
- Perceptual difficulties, such as distance estimation.
- Depression, anxiety, and irritability are mood changes.
Middle Stage Dementia
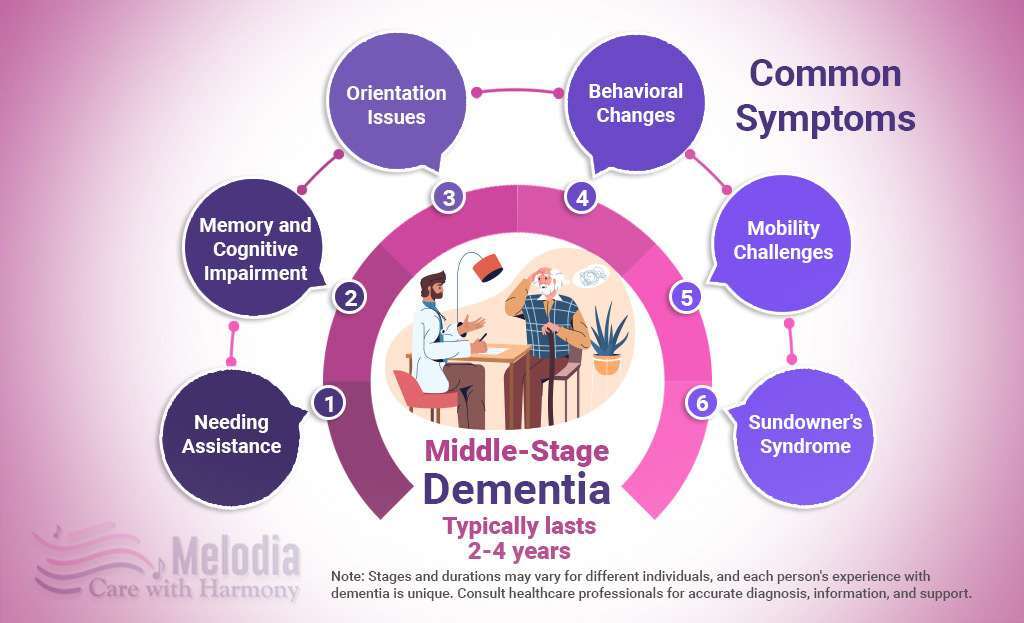
The middle stage of dementia lasts about 2–4 years. It’s generally the longest.
Middle Stage Dementia Symptoms Include:
- Needing a caretaker for tasks like cleaning and dressing
- Difficulties recognizing loved ones, trouble recalling facts, trouble following talks
- Increasing orientation issues, such as getting up and dressed mid-night, developing false beliefs, and experiencing paranoia.
- Changes in behavior, such as screaming, anger, poor sleep, and repetitive activity
- Mobility difficulties, difficulty using the toilet
- Sundowner’s syndrome, when the person becomes anxious and worried in the late afternoon, is a common symptom of middle-stage dementia.
Late Stage Dementia
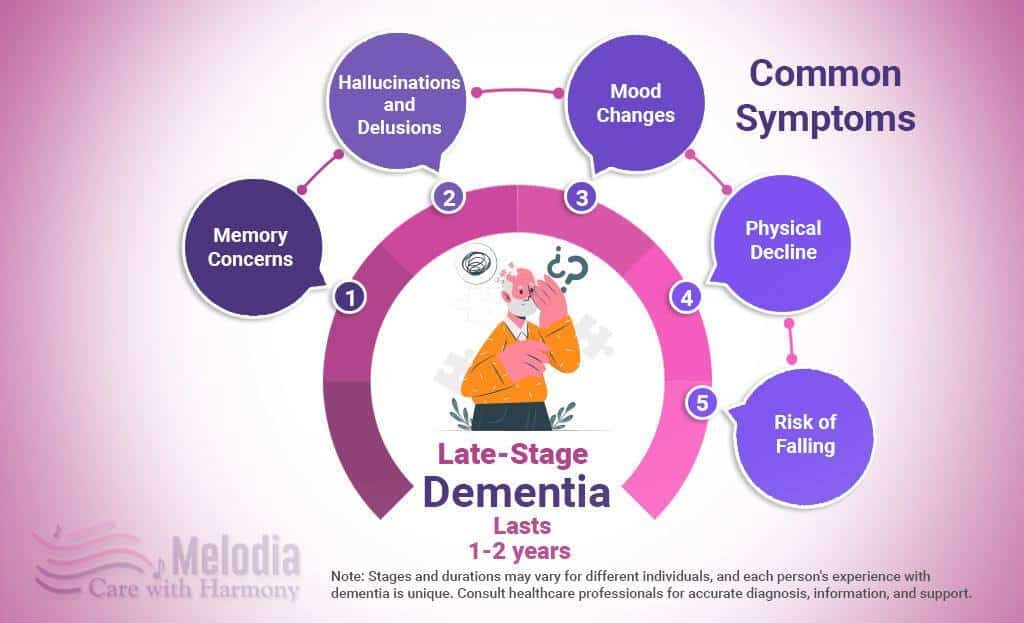
Late-stage dementia patients may need 24-hour care from caregivers. The final stage lasts 1–2 years, depending on age and health.
Late Stage Dementia Symptoms include:
- Memory concerns, such as time-shifting, where a person thinks they are at an earlier moment and cannot recognize loved ones or themselves. Language issues, such as understanding fewer words
- Hallucinations and delusions
- Changes in moods, such as despair and apathy, aggression due to fear, threat, and confusion
- Trouble walking and needing more time sitting or in bed; difficulty swallowing and needing significant help with eating; incontinence (losing control of their bowels); weight loss
- Risk of falling
How Does Dementia Reduce Life Expectancy?

Many dementia-related disorders diminish life expectancy. Some of these are:
- Diabetes
- Heart disease
- Stroke
Dementia impairs the immune system, and people with dementia typically have trouble swallowing. This increases their risk of additional medical disorders, such as:
- Brain blood clots
- Lung blood clots
- Pneumonia
How to Care For Someone With Dementia

Dementia can be difficult for family and friends. The U.S. Department of Health and Human Services offers dementia caregiver tips.
- Maintain a dementia-friendly schedule. This includes daily bathing, eating, and dressing.
- Plan and encourage them to dance or exercise.
- To-do lists, notebooks, and calendars can help a person stay organized and in charge of their daily routine.
- When performing activities with them, Give them as much control as possible.
- Always be constant and familiar.
- Choose zips and elastic waistbands over buttons, belts, and shoelaces.
- Respect their privacy and let them run their lives.
- Provide comforting photos and objects.
- Listen to grievances without judgment.
- Remove carpets they may trip over and store chemicals they may misinterpret to make their home safer.
How Can Patients Be Discharged From Hospice?

Hospice care is no longer available if a patient’s condition improves, treatment may be restarted, or their life expectancy exceeds six months.
A hospice patient may be released for reasons other than their terminal condition. Hospice patients can leave at any moment for any reason. When patients opt out of hospice care, they lose all Medicare Hospice benefits, including home medical equipment, supplies, home visits, and therapeutic or holistic services.
A hospice patient may relocate out of the service area or need to transfer to a different hospice. A patient may be discharged if their behavior is disruptive, uncooperative, or abusive enough to hinder hospice care. Patients can challenge hospice discharges.
If a hospice patient’s condition worsens after discharge, they can be readmitted.
Contact the Melodia Hospice Care Staff
Do you have a family member with Alzheimer’s? Do you think it is time to enter hospice care? Discuss why with your loved one’s physician and home health care team. Skilled dementia care professionals from Melodia Hospice Care can provide information on this matter.








