Bile duct cancer is an uncommon but deadly disease that affects the bile ducts.
The bile duct, often known as the “bile duct system,” is a network of tubes that runs from the liver to the small intestine. Bile is a digestive fluid that helps the body break down fat and digest meals.
Cancer that has progressed to the exterior of the bile duct is known as advanced bile duct cancer. It might also refer to cancer that has returned after the initial therapy. Recurrent bile duct cancer is the name for this type of malignancy.
Unfortunately, by the time bile duct cancer is detected, most patients already have advanced cancer. This is due to the fact that bile duct cancer frequently has no early signs. When it does develop symptoms, they might be confusing and difficult to identify.
The following are the several types of advanced cancer:
Bile duct carcinoma that has progressed locally
Cancer of the bile duct that has spread throughout the body like in the lungs.
The term “locally progressed” refers to cancer that has spread to lymph nodes or organs near the bile ducts. Bile duct cancer normally progresses along the bile duct in a localized manner.
Localized bile duct cancer may have spread to the liver and small bowl pancreas or in the vicinity of a major blood vessel.
This might indicate that surgery is not a viable option at this stage. This type of cancer is referred to as inoperable cancer by doctors.
Cancer that has spread to another section of the body is referred to as secondary or metastatic cancer. This indicates that the cancer has progressed through the circulation or lymphatic system to more distant organs.
The following are the most typical sites where bile duct cancer spreads:
- lungs
- Bone
- Peritoneum (lining of the abdomen)
- pleura (lining of the lungs)
You would undoubtedly scared and apprehensive about the future. It’s impossible to think of anything else when you’re dealing with cancer.
Reports shows that dealing with advance cancer makes difficult for you to comprehend ordinary events or daily life activities like before.
You must set priorities. Consider how you want to spend your time, as well as what is and is not essential to you. Some of your future ideas might no longer be feasible, but you don’t have to abandon them entirely. Perhaps you could personalize something. And perhaps you can always accomplish what you wanted to do but couldn’t because of a lack of time.
End-of-life care is to help you live a quality of life until you die, and to do so in a dignified manner.
End-of-life care refers to the treatment of persons in their final months or years of life. End-of-life care must begin as soon as possible and may take days, months, or even years.
End-of-life care may help people in a number of scenarios. Some are predicted to pass away within the following several hours or days. Others are cared for months as they approach the end of their life.
People who are towards the end of their lives are expected to die within the following 6 months, although this is not always the case. Those who are dying, as well as those who:
Cancer, dementia, and motor neuron disease are examples of advanced incurable illnesses.
There are several terminal illnesses that can make more likely to die within a year.
Have a pre-existing medical condition that puts them at danger of dying in the event of a rapid deterioration of their condition.
Have a life-threatening acute condition as a result of a sudden catastrophic occurrence.
Death is accepted as the last stage of life in the hospice concept. It acknowledges life without attempting to hasten or postpone death. Hospice care focuses on the person’s and the illness’s symptoms rather than the sickness itself. A team of professionals will collaborate to manage the symptoms while they are surrounded by loved ones, allowing them to spend their final days in dignity and comfort. Hospice care is also centered on the family, with patients and their families participating in decision-making end-of-life.
Stages Of Bile Duct
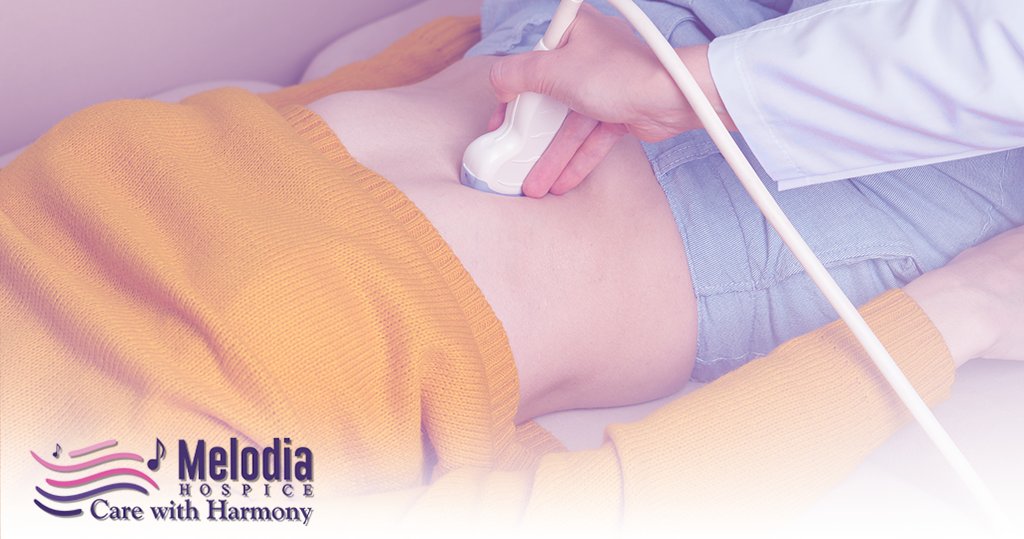
The staging system is the most common method used by cancer treatment teams to summarize the degree of the cancer. The TNM classification of the United States Joint Commission on Carcinoma (AJCC) is the most widely used approach for describing the stage of bile duct cancer. There are three alternative staging methods for bile duct cancer, depending on where it arises.
- Cholangiocarcinoma of the liver (intrahepatic cholangiocarcinoma) (occurs in the liver)
- Bile duct carcinoma in the peri-hilum (occurs in the hepatic hilum, the area just outside the liver)
- The distal bile duct carcinoma is a kind of cancer that affects the bile duct (starting further below the bile duct system)
Almost all bile duct cancer starts in the innermost layer of the bile duct wall, which is referred to as the inner layer. They can grow through the walls of the bile ducts to the exterior over time. The tumor can invade (grow) surrounding blood vessels, organs, and other tissues when it develops through the walls of the bile ducts. It can also spread to surrounding lymph nodes and other regions of the body by growing into nearby lymph and blood arteries.
Doctors strive to determine if bile duct cancer has spread and, if so, how far it has gone after a person is diagnosed. This is referred to as staging. The cancer stage refers to how much cancer is present in your body. It aids in determining the severity of the malignancy and the best treatment options. Cancer staging is frequently used by doctors when evaluating survival rates.
Stage 0 is the first stage of bile duct cancer (also known as carcinoma in situ or CIS). The stage will thereafter be in the range of stage I (1) to IV (4). The lesser the number, the less likely the cancer will spread. A greater number, means the dangerous the cancer is.
Stage IV indicates that the cancer has progressed to an incurable level. Despite of the fact that each person’s cancer experience is unique, cancers at similar stages tend to have similar outcomes and are frequently treated in the same way.
Physical examination, biopsy, and imaging data are used to assign a clinical stage to bile duct cancer. The pathological stage (also known as the surgical stage) is assessed during surgery by evaluating the tissue removed during the procedure.
Symptoms Of Bile Duct Cancer
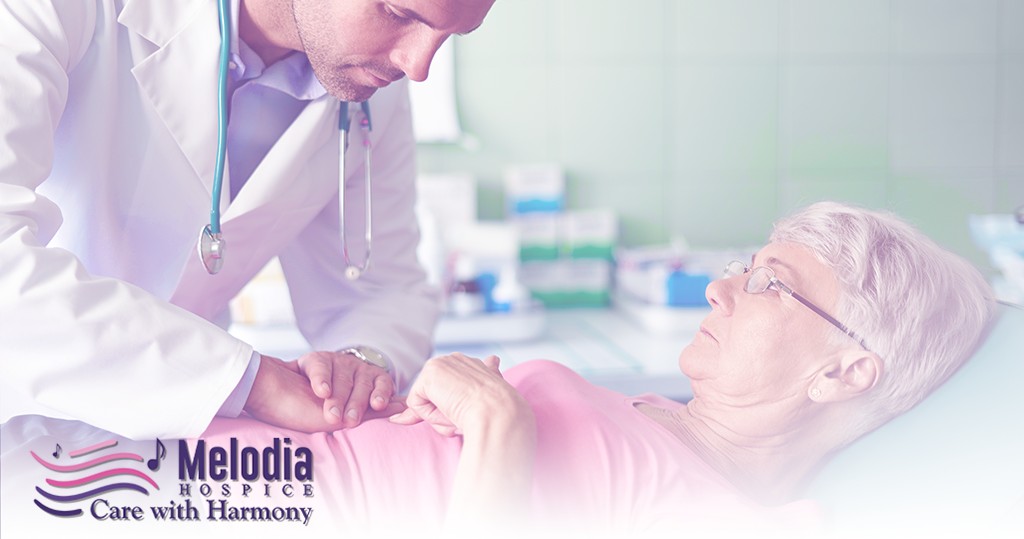
Symptoms of bile duct cancer normally do not appear until the liver’s bile flow is obstructed.
In most cases, the illness has progressed to an advanced stage. Bile flows back into the blood and tissues of the body as a result of the blockage, giving the following symptoms:
Jaundice is characterized by skin yellowing, white eyes, itchy skin, pale stools, and black urine.
Weight Loss That Isn’t Intentional
Most persons complain of a dull discomfort in the upper right region of their abdomen
High temperatures exceeding 38 degrees Celsius (100.4 degrees Fahrenheit) and chills
Appetite decreases
What Causes Bile Duct Cancer?

It is uncertain what causes bile duct cancer. Certain factors, though, can raise your chances of having a disorder. The most common is being over the age of 65, or having a rare chronic liver illness known as primary sclerosing cholangitis (PSC).
Different types of bile duct cancer
Depending on where the cancer starts, there are two forms of bile duct cancer.
- Intrahepatic bile duct carcinoma is cancer that originates in a portion of the liver’s bile ducts.
- Extrahepatic bile duct cancer is cancer that starts in a section of the bile duct outside the liver.
diagnose
Bile duct cancer can be difficult to detect and may necessitate a number of tests, including:
- examination of the blood
- Ultrasound examination
- CT (computed tomography) scan
- MRI (magnetic resonance imaging) scan
Some of these tests necessitate the injection of a specific dye that highlights the bile ducts. A biopsy may also be necessary. Microscopic examination of small tissue samples is performed. In other circumstances, however, surgeons may decide to remove a suspected tumor based only on the scan results.
A Biliary Stent Or A Biliary Catheter Are Also Options

If cancerous cells obstruct a bile duct, it can result in jaundice (yellowing of the skin and eyes), as well as other issues include pollution and liver failure. A tiny tube or catheter may be inserted into the duct to help keep it open.
A stent is a tiny metallic or plastic tube that is inserted into the duct through the blockage. It keeps the duct open, allowing bile to empty into the small intestine.
A catheter is a thin, bendy tube that is inserted through the skin of the abdomen (belly). One end of the tube is inserted into a bile duct, while the other end is implanted outside the body.
Treatment Options
A group of doctors and other specialists will meet to determine the best course of treatment and care for you.
They are referred to as the Interdisciplinary Team (MDT).
If you have advanced bile duct cancer, surgery to cure the cancer is not an option. Other treatments that slow or slow growth may exist, though. This will help you control your symptoms and make you feel better.
The best treatment for you is determined by the following factors:
Cancer is spreading
Secondary cancer size and number
Your general health
Your symptoms and the treatment you’ve already received
Your desire.
You can reach Melodia Care at any time of day or night by contacting us through our 24/7 online customer support chat or by calling 1-888 635-6347 (MELODI-7).










