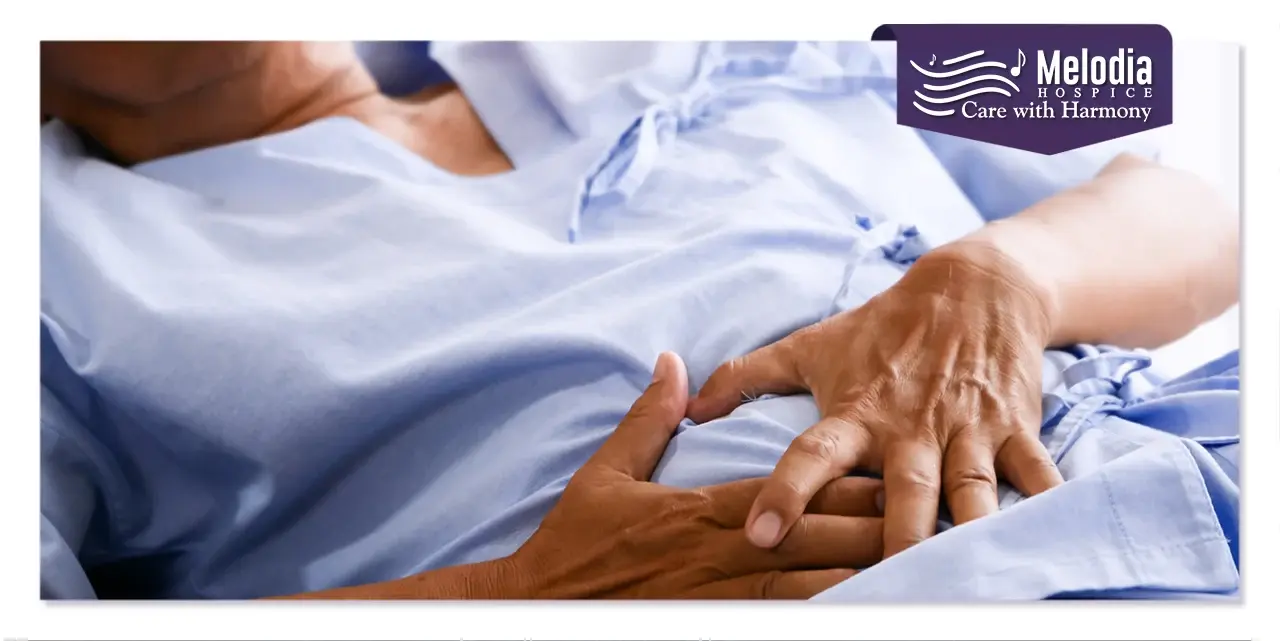
Advanced Stage IV Esophageal cancer is a disease in epidemiologic transition. Patients with stage IV esophageal cancer have metastatic cancer. In Stage IV, esophageal cancer has spread to distant parts of the patient’s body. These patients have many complex symptoms, including:+
- Pain
- Dysphagia
- Malnutrition
- Psychological symptoms due to the location of the tumor and the treatment required
The advanced prognosis of esophageal cancer forces caregivers and relatives to discuss concerns with the medical team and seek professional help. Palliative care is a medical care subspecialty focused on providing comprehensive care for patients with any advanced or severe disease so that they can live as comfortably as possible while facing this disease. Patients with advanced esophageal cancer who are expected to live less than six months may be eligible to receive hospice care in hospitals or other healthcare institutions or individual homes. Hospice care only provides pain management and palliative care and does not treat esophageal cancer itself.
Early Symptoms & Signs of Esophageal Cancer
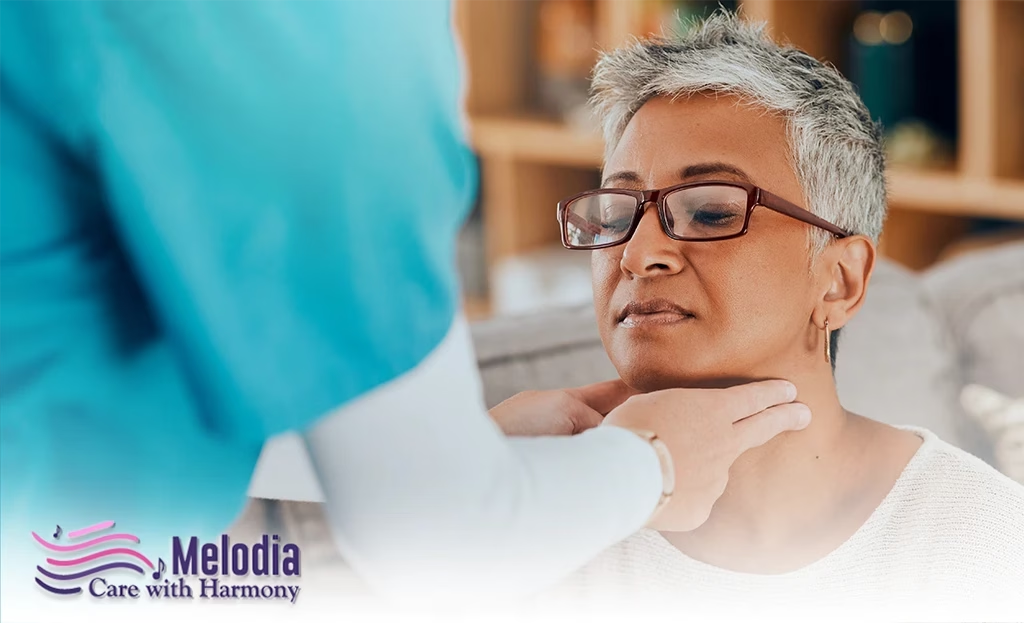
In the early stage, esophageal cancer usually has no apparent signs or symptoms. When they do appear, the most common symptom is difficulty swallowing. Regularly eating bite-sized foods may make you feel like you’re choking or something is stuck in your throat.
Other early signs and symptoms may include:
- Weight loss
- Chest pain
- Heartburn or indigestion
- Hoarse voice
- Cough
Signs & Symptoms of End-Stage (Stage Iv) Esophageal Cancer

As the disease progresses and the cancer metastasizes, esophageal symptoms tend to worsen. For example, dysphagia may reach the point where a pure liquid diet is required.
Other advanced signs and symptoms of esophageal cancer may include:
- Increased cough and sore throat
- Difficulty breathing
- Hoarseness
- Hiccup
- Nausea and vomiting
- Bone and joint pain
- Infection in the digestive tract because of bleeding in the esophagus
- Fatigue, which may be caused by anemia caused by blood loss; certain medications and cancer treatments; poor sleep due to pain or medication side effects
Palliative Care for Patients With Stage Iv Esophageal Cancer
It is recommended that all cancer patients undergo palliative care at the same time as cancer-oriented treatment-regardless whether the cancer treatment is to cure or to control the spread of the disease and prolong life. There are two levels of palliative care for cancer patients.
- Primary Palliative Care
- Specialist Palliative Care
Primary Palliative Care
Primary palliative care is symptom management and nursing dialogue provided by the patient’s primary oncology team. It is the first layer and applies to all cancer patients. For patients with complex needs, referral to palliative care specialists is recommended.
Specialist Palliative Care
Specialist palliative care is best provided by an interdisciplinary team of professionally trained physicians, nurses, social workers, pastors, and pharmacists who work with the patient’s typical healthcare provider to provide comprehensive symptom management, psychosocial and spiritual support and advance care planning. Given the shortage of professional palliative care providers, this two-tier approach is essential.
Importance of Hospice Care for Patients With Stage 4 Esophageal Cancer
When a healthcare team determines that cancer can no longer be controlled, they usually stop medical testing and cancer treatment. But patient care continues, focusing on improving the quality of life of the patient and their loved ones and making them feel comfortable in the next few weeks or months. The medications and treatments people receive when dying can control pain and other symptoms, such as constipation, nausea, and shortness of breath. Some people stay home while receiving these treatments, while others go to hospitals or other institutions. Either way, these services can help patients and their families solve medical, psychological, social, and spiritual problems related to death. The hospice is the most comprehensive and coordinated provider of these services. Everyone’s end-of-life period is different. People’s signs and symptoms may vary and each individual has unique requirements when it comes to information and support. Family members should discuss issues & concerns related to death with each other and with the medical team when they arise. In the last few months of a person’s life, communication about hospice care and decision-making is very important. For cancer patients, it is essential to make these decisions before they are too sick to make these decisions. However, if a person does become very ill before completing the advance instructions, it is helpful for home caregivers to know what type of care their loved ones would want to receive.
When You Should Seek Professional Help?

In any of the following situations, caregivers can contact the patient’s doctor or nurse for help:
- The patient’s pain cannot be relieved by prescribed doses of pain medication.
- The patient develops new symptoms such as nausea, vomiting, confusion, anxiety or irritability.
- The patient shows discomfort, such as making faces or moaning.
- The patient has difficulty breathing and looks very disturbed.
- The patient is unable to urinate or defecate.
- The patient is very depressed or talks about suicide.
- It is difficult for caregivers to provide medication to patients.
- The caregiver is overwhelmed by caring for the patient and is too sad or afraid to be with the patient.
- The caregiver does not know how to deal with a situation
What Are Some Ways to Provide Emotional Support for Cancer Patients?

Everyone patient has different needs, but most dying patients have some concerns. Two of these concerns are fear of being abandoned and fear of becoming a burden. Dying people also worry about losing their dignity and control.
Here are some ways that caregivers can provide comfort to people with such concerns:
- Keep in touch with this person. Talk to them, watch a movie with them, read a book with them, or be with them.
- Allow patients to express their fears and worries about death, such as leaving family and friends. Get ready to listen to them.
- Willing to recall this person’s life.
- Avoid hiding important information. Most patients prefer to participate in discussions about issues related to them.
- Assure patients that you will follow advanced instructions, such as a living will.
- Ask if there is anything you can do.
- Respect the needs of individuals for privacy.
- Support people’s spirituality. Let them talk about what makes sense to them. If they want, you can pray with them and arrange visits for spiritual leaders and church members where appropriate. Keep items that are meaningful to them at hand.
Treatment Methods to Relieve the End-Stage Symptoms of Esophageal Cancer
Treatment methods to relieve the pain and discomfort of terminal symptoms include medication and surgery.
It is essential to discuss the pros and cons of each option because specific treatments may interfere with a person’s quality of life or dying wishes.
Esophageal Dilatation
If swallowing becomes too difficult, dilatation of the esophagus may be an option. During this process, the doctor stretches a small balloon-shaped cylinder down into the esophagus, which gently stretches the tissue and expands the opening to allow food and liquid to pass through. Another similar procedure involves placing a stent in the esophagus to keep it open.
Laser Ablation
The doctor may also use a laser beam to target the cancerous tissue that narrows the esophagus. The light beam destroys tissues and improves swallowing and digestion.
Feeding Tube
If the procedure to enlarge the esophagus is unreasonable or unpopular among patient or their family, the doctor may insert a feeding tube. The feeding tube provides nutrition directly to the blood vessels or stomach or small intestine. This is done to prevent malnutrition and extend life expectancy. Although they are more common in hospitals or hospice settings, some feeding tubes can be used at home. Palliative care nurses can provide instructions on how to handle the feeding tube.
Analgesics
To relieve pain and other symptoms, for example, if swallowing a pill is too difficult, doctors will provide various drugs and methods to deliver these drugs.
Analgesics are divided into two main categories:
- Opioids
- Non-opioids
In recent years, opioids such as fentanyl and oxycodone have received considerable attention due to their addictive properties and the tragic stories of people who abuse these drugs. However, if used properly and under strict supervision, opioids can effectively treat the pain of advanced cancer and other diseases. When non-opioid pain relievers such as ibuprofen (Advil) and acetaminophen (Tylenol) are ineffective, they are usually prescribed.
(FAQs)
What is stage 4 esophageal cancer?
Stage 4 esophageal cancer is the most advanced stage of the disease, characterized by the cancer’s dissemination to distant regions of the body, including the liver, lungs, or bones.
What are the symptoms of stage 4 esophageal cancer?
Common symptoms of stage 4 esophageal cancer include coughing, fatigue, weight loss, and difficulty swallowing.
What is end-of-life care?
End-of-life care is a type of care that is dedicated to alleviating pain, enhancing the quality of life, and providing comfort to patients with a terminal illness.
What are the advantages of hospice care for stage 4 esophageal cancer?
Hospice care provides various advantages, such as enhanced symptom management, increased patient and family satisfaction, more comprehensive support for patients and their families during the end-of-life journey, and an improved quality of life.
Conclusion
The signs of death from esophageal cancer are similar to those experienced by patients with other types of cancer. It is usually possible to relieve pain and general weakness of the body while slowing down all bodily functions with powerful drugs. Symptoms of esophageal cancer, such as difficulty swallowing, will gradually worsen so that a feeding tube may be required. Although physical pain is usually manageable, the emotional and spiritual challenges experienced by cancer patients, their friends, and family members are sometimes more challenging to control. Focus on providing support and taking steps to ensure their physical comfort. And don’t hesitate to talk to palliative care providers to get their opinions and suggestions.
You can reach Melodia Care at any time of day or night by contacting us through our 24/7 online customer support chat or by calling 1-888 635-6347 (MELODI-7).